Swollen Eyes And Eyelids: Why And How To Treat Them
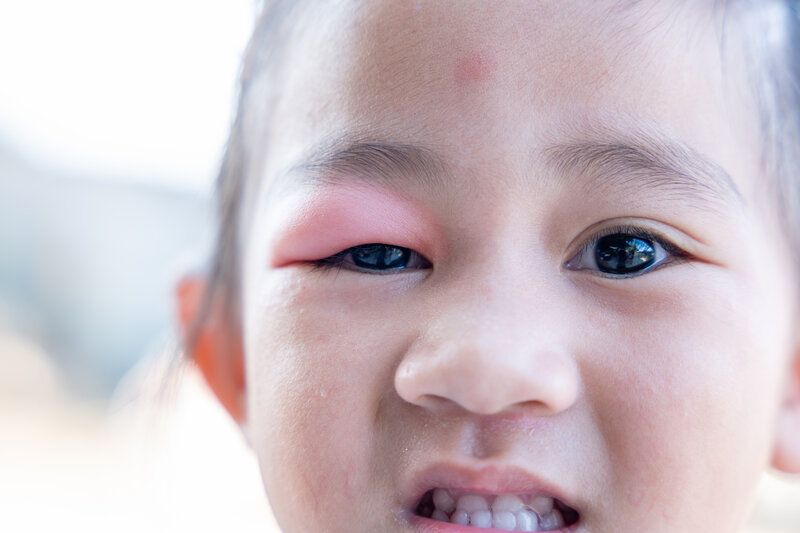
Spring is here, and everything is blooming and blossoming out, which means our office is flooded with calls regarding swollen eyes and eyelids. In most cases, inflamed tissue in and around the eyes is caused by allergies or the irritation caused by foreign objects. However, there are cases where eye tissue becomes infected, in which case you’ll need to visit your optometrist.
Inflammation Of The Eye And Eyelids
Here are some of the most common reasons the membranes in the eyes, eyelids, or the tissue surrounding the eyes become red, swollen (inflamed), or irritated. And remember - resist the urge to rub your eyes, especially when they’re red or inflamed, as rubbing can make the situation worse and lead to scratched corneas.
Allergies can cause swollen eyes and eyelids
Pollen, pet dander, and mold spores are three of the most common causes of eye allergies. This time of year, all are in abundance as grass, and flowering plants begin to bloom, increased warmth inspires the release of mold spores, and pets shed more dander as they trade their thicker coat in for their summer coat.
Any airborne particulates can get into the eyes, and if you’re allergic, they wreak havoc. Your eyes may get red and watery. They often itch, and you may even see the outer membrane of the eye (the sclera) bubble up like a small water balloon - causing further discomfort.
Over-the-counter allergy eye drops and allergy medication are your best lines of defense. First, speak to your physician if you feel allergies are causing inflammation of the eyes and eyelids, and then be diligent about taking physician-approved allergy medication. If that doesn’t clear things up, call your optometrist, and they’ll provide further instructions.
Blepharitis (inflamed eyelids)
Blepharitis, or swollen eyelids, is most commonly experienced along the edge of the upper- or lower lids. It’s caused by bacteria that become trapped in the eyelash follicles, causing swelling and irritation. While anyone can develop blepharitis at any time, it’s most likely in those with dry skin (dandruff), rosacea, or oily skin. Blepharitis can also occur when the microscopic mites that live in your eyelash follicles become overpopulated.
In most cases, blepharitis resolves on its own. However, to provide relief and to help it clear up faster, we recommend applying a warm, moist compress for at least a minute at a time. Use a clean soft washcloth, wet it with warm water, wring it out until it’s almost dry, and then fold it and place it over your eyes. Moisten it as often as you need to until the dry, flakey crust residue is gone.
It’s important to wash your eyes well each day to keep eyelash follicles free of dirt, skin, bacteria, and oil buildup. If your blepharitis doesn’t clear up within a few days or it becomes worse, contact your optometrist.
Stye
Styes are similar to blepharitis but they are not the same. While blepharitis affects the entirety of the eyelid, a stye only affects one or two follicles, leading to a red, painful, and irritating bump on the edge of your eyelid. They’re most common on the lower lid but can occur on the upper lid as well.
A stye is caused by an infected eyelash follicle or oil gland. In some cases, they develop a white head just like a pimple or clogged pore on the face or body. Resist the urge to pop or squeeze a stye as you can make it worse or it can develop into a more severe infection. Instead, use warm moist compresses to provide soothing relief and to encourage the clogged or infected follicle/gland to drain.
As with blepharitis, styes typically clear up on their own within a week or two, although residual redness and swelling may last up to three weeks. If the stye worsens or you aren’t feeling relief after two weeks, schedule an appointment with the eye doctor.
Uveitis
When you have eye allergies or surface irritants in the eye, your sclera can bubble up. The layer beneath the sclera is called the uvea (yoo-vee-yah). Inflammation of the eye’s uvea is called uveitis and requires immediate attention as chronic uveitis can eventually impact your vision.
Keratitis
If your cornea is injured, it can become inflamed. We call this keratitis. Like other infections, keratitis occurs when bacteria, viruses, or parasites get into scratches or tears in the cornea. You’re more likely to develop keratitis if you’ve recently experienced eye trauma, you have dry eyes, or you over-rub your eyes.
Bacterial or viral eye infections
Anytime your eye is infected, inflammation of the eye and lids is sure to follow. Unlike allergy-related inflammation, bacterial or viral eye infections typically involve goopier eyes (white, yellow, or green discharge) in addition to redness, irritation, excessive tearing, and light sensitivity.
Because eye infections are highly contagious, we recommend checking in with your eye doctor or physician. In most cases, we’ll want to take a look to determine the cause of the infection (bacterial or viral) so we can prescribe the right drops or ointment. Most eye infections begin to clear up within 24-hours of using prescription drops.
Thyroid eye disease (TED)
Sometimes called Graves’ ophthalmopathy or Graves’ Eye Disease, thyroid eye disease (TED) is an autoimmune disorder. If the immune system mistakenly attacks tissues in or around the eye, it causes inflammation of the eyes and eyelids. It’s common for patients who have overactive thyroids.
If you’ve already been diagnosed with hyperthyroidism, your physician and optometrist will keep a close eye on your vision and the health of your eyes to catch any episodes of TED and treat them to minimize damage to the eyes. In some cases, chronic eye inflammation triggers a referral from us to your physician to identify whether an overactive thyroid may be the cause.
Never Hesitate To Contact Us Whether It's Swollen Eyes And Eyelids Or Anything Else
The team at Eye to Eye Family Vision Care is here to listen to your concerns and answer any questions. Please feel free to give us a call at, 918-227-3937, or schedule an appointment so we can identify the cause of your eye inflammation or irritation. Swift identification is key to faster treatment, healing, and restored comfort.

